Update 16 Sep 2009: Last year’s $211 million figure for taxpayer-funded obstetric care, mostly of pregnancies and births that are or could have been normal, has blown out further to $298 million. [Via the Courier Mail.]
~~~
The Maternity Services Review is finally out. But you knew that, because last week the Australian Medical Association published a badly flawed paper designed to suggest that private obstetric care was the only safe way to birth a baby.
And the buzzword for today is: “collaborative care”. In other words, “The Maternity Services Review report was written by a committee, which panicked under lobbyist pressure and didn’t actually want to commit to anything at all”.
You can find the Review here:
Improving Maternity Services in Australia : The Report of the Maternity Services Review, February 2009
The review was led by Rosemary Bryant, Commonwealth Chief Nurse and Midwifery Officer. Note that Ms Bryant is not, nor has she ever been, a midwife.
I’ve picked out a few bits from the context and discussion parts of each section to talk about, and provided the full text of the Conclusions and Recommendations for all sections. If you’re interested in the subject, do read the whole thing; this doesn’t pretend to be a comprehensive summary, just my 2 cents worth of nitpicking, ranting and raving. I haven’t looked at news reports yet. This is my bare response. And you’ll only find out about my headline if you read all the way to the end. Ha!
1. Safety and Quality
There seem to be errors in the first two Figures, one of them major and misleading. I don’t know how many other errors of fact there are in the report, but this is obviously a concern.
Figure 1 claims to show the “Number of women who die in childbirth, Australia, 1991-2006”.
However, from the text, it seems that this is actually a graph of direct maternal mortality, not a graph of deaths in childbirth. Maternal mortality is defined as any death from conception to 42 days postpartum, and it’s divided into Direct (eg eclampsia), Indirect (exacerbated by pregnancy, eg cardiac failure, psychiatric illnesses), and Incidental (eg car accident). (Maternal mortality statistics collection has recently been extended to include a category of late maternal deaths – deaths from direct or indirect causes that may occur up to a year after the birth.) The Direct category does not only include deaths in childbirth, it includes all deaths directly related to complications of pregnancy, birth, or the postpartum period in some way. They therefore include deaths from conditions like ectopic pregnancy, hypertensive diseases of pregnancy, pulmonary embolism, antepartum haemorrhage, and postpartum infection or haemorrhage.
I’m finding it difficult to have a lot of faith in a report written by someone who is unfamiliar enough with maternity care that the basics about maternal mortality statistics are off, so we’re not off to a good start. Maybe we’ll find out this was the fault of a subeditor?
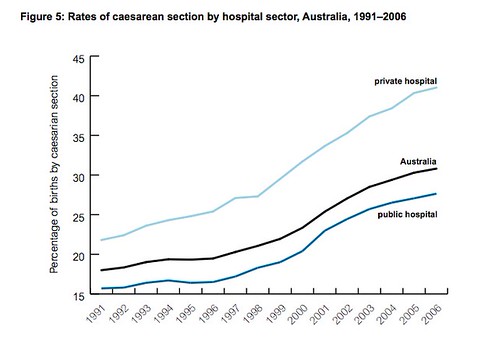
The point I’d like you to note about this graph is that it shows that maternal mortality hasn’t improved from 1991 to 2006, though major intervention rates have skyrocketed over that time. Here’s the C section rate.
The other error is a date typo in Figure 2. This is not a major drama once you realise that “1996” is supposed to be “1966”, but it speaks to poor quality control.
Firstly, note that this infant mortality graph isn’t on the same timescale as the first graph, which starts at 1991. If you start at 1991, infant mortality has barely changed from then to now, despite all the “we saved the baby!” C sections that have been done. The biggest drop in infant mortality occurred in the 1970s.
What these graphs don’t show, but it is discussed in the text, is the abysmal mortality figures for Indigenous women and babies. Maternal mortality for Aboriginal and Torres Strait Islander women runs two to five times the mortality for white women in Australia, and infant mortality is doubled to tripled. Yet this large-scale national disaster doesn’t get anywhere near the mainstream media time that the AMA’s posturing about turf wars gets.
The report briefly acknowledges that some submissions emphasised the need to take into account more than maternal and perinatal mortality alone when planning maternity care services; and briefly acknowledged the existence of debate over medically appropriate intervention rates.
Conclusions
The Review Team concluded that:
* Australia’s strong record of safety in maternity services is an acknowledged strength of our maternity system.
* Changes to maternity services need to be guided by evidence.
* Stable, ongoing arrangements for national maternity data collection, analysis and review must be a priority.
Recommendations
1. That the Australian Government, in consultation with states and territories and key stakeholders, agree and implement arrangements for consistent, comprehensive national data collection, monitoring and review, for maternal and perinatal mortality and morbidity.
2. That the Australian Government, in consultation with states and territories and key stakeholders, initiate targeted research aimed at improving the quality and safety of maternity services in select key priority areas, such as evidence around interventions, particularly caesarean sections, and maternal experience and outcomes, including from postnatal care.
2. Access to a Range of Models of Care
Immediately the authors move away from their claimed commitment to an evidence-based model, toward what is politically expedient. They had an opportunity here to mention The Cochrane Collaboration’s evidence-based review of models of care, and the World Health Organisation’s information on Safe Motherhood, which they ignored. Instead, we have this:
In recognising that, at the current time in Australia, homebirthing is a sensitive and controversial issue, the Review Team has formed the view that the relationship between maternity health care professionals is not such as to support homebirth as a mainstream Commonwealth-funded option (at least in the short term). The Review also considers that moving prematurely to a mainstream private model of care incorporating homebirthing risks polarising the professions rather than allowing the expansion of collaborative approaches to improving choice and services for Australian women and their babies.
Why is a government report designed to stimulate rational national reform backing away from “sensitive” issues? Could it be that it’s not actually there to stimulate reform at all?
The report notices that some women are choosing to freebirth (birth without a healthcare practitioner present).
Of concern to the Review Team is the number of submissions and other evidence that suggests a small number of Australian women are choosing homebirths without the support of an appropriately trained health professional. Accordingly, as with any other maternity care model, the Review Team considers that appropriate standards, monitoring and evaluation should be integral components of any service involving homebirth.
This is noted with expressions of deep concern, but the context of freebirthing remains completely unexplored. That context is lack of access to midwifery care. Many (though not all) women who freebirth do so because the choice they wish is simply not available to them. And that choice – accessible, affordable, midwife-attended, woman-centred homebirth – certainly isn’t going to become any more available as a result of this report.
I note that the issues of non-consensual intervention, violence and birthrape at the hands of birthing practitioners is not mentioned. “Consent” is absent. The only violence present is domestic violence. Women’s experiences are erased. And the only women with “culture” are Indigenous women. References to Indigenous culture is placed in a special section (see 3.2), and plucked out of submissions and forum contributions in a way that simultaneously Others and distances them from from the “default”, and completely erases the cultural context of birthing for non-Indigenous women:
The birthing experience of Aboriginal and Torres Strait Islander women is fundamentally culturally different from that of non-Indigenous women. Birthing is and continues to be – in some communities – a cultural rite of passage where knowledge, practices and beliefs are transferred from older to younger women, identity and links are established to land and connections with country are shared and celebrated.
[…]
There are 3 key elements of Alukura’s underlying philosophy. Firstly, it acknowledges that Aboriginal peoples are distinct and viable cultural groups with our own cultural beliefs & practices, law & social needs. Secondly, it recognises that every woman has the right to participate fully in her pregnancy & childbirth care, and determine the environment and nature of such care. Finally, it recognises that every Aboriginal woman has the right in pregnancy and childbirth to maintain and use her own heritage, customs, language and institutions.
Where is the “fundamental” difference here? Aboriginal and Torres Strait Islanders absolutely need to have access to culturally appropriate and community-controlled services in which their cultural, spiritual, and social context is respected and celebrated. This does not make their needs “fundamentally” different from birthing white women. There is no need to exoticise and set aside culturally-appropriate birthing as an optional nice extra, something a little bit ‘primitive’, something a little bit strange and difficult to understand and not “Us”.
Models of Care Conclusions
* The Review Team concluded that: Continuity of care relies on the ability of practitioners to work together and on the capacity of services to link together as the woman moves through pregnancy to childbirth.
* Greater choice in maternity care could be provided by collaborative care models, which draw on the expertise of the range of health professionals involved in maternity care.
* It is clear that increased choice for women could be provided if there were greater recognition of the role that midwives can play in collaborative care models.
* Options should be explored for increasing the availability of birthing centre programs.
* Interdisciplinary national guidelines for maternity care that are agreed by the relevant professional disciplines would support the maternity care team in the provision of safe, quality, collaborative care for women and their babies.
Recommendations
3. As a priority, that the National Health and Medical Research Council (NHMRC) develop national multidisciplinary guidelines for maternity care to promote consistent standards of practice, quality and safety in collaborative team models. These guidelines are to be agreed by the professions involved, in consultation with consumers and state and territory governments.
4. That, in developing the National Maternity Services Plan, consideration be given to the demand for, and availability of, a range of models of care including birthing centres.
3. Inequality of Outcomes and Access
3.1 Rural
Conclusions.
The Review Team concluded that:
* Mechanisms to improve maternity care networks so that systematic processes exist to link local, regional, and tertiary services with support and backup are vital.
* Collaborative care models developed for rural communities must reflect local circumstances, including the availability of appropriately skilled workforce.
* The role of outreach services is an important component of the service mix.
Recommendation
5. That, given the role of the states and territories in the provision of maternity services in rural areas, the availability of rural maternity services is a priority area for the Plan, requiring the engagement of states and territories.
3.2 Indigenous
The massively disproportionate burden of illness and mortality in the Indigenous population is noted. There is a desperate need to improve many aspects of Indigenous healthcare determinants, and direct maternity healthcare provision only a tiny part of this. This report looks at health very much in terms of a very biomedical “risk factor” model, referring to smoking, substance misuse, poor nutrition, poor dental health and domestic violence. There is little or nothing about the larger determinants: dispossession, spiritual and cultural dislocation, poverty, institutional prejudice and paternalism, community direction and control.
This Maternity Services Review doesn’t talk about this, but the Rudd government’s “closing the gap” lip-service campaign seems to be grinding its gears, and the promise of the Apology is but a whispered echo only a year later.
The report does place an emphasis on the need for culturally appropriate community-based maternity care models under the control of local women, some of which may be midwife-led services. This demonstrates that the MSR is capable of thinking in a woman-centred way that takes into account cultural beliefs and women’s feelings of safety – but they only choose to do so when it’s politically convenient, because no-one in power is after that “turf”.
Why are obstetricians so keen to retain complete control over white urban women’s maternity care “because it’s the safest way”, but are happy (perhaps thrilled) to relinquish the care of Indigenous women to the midwifery-led and community-controlled services they revile? This issue, more than any other, I think, exposes OB hypocrisy for what it is: territory wars and financial interest, not ideas of maternal safety. Poor Indigenous women don’t live in places where obstetricians want to practise, and they don’t have the money to pay. So they’re an afterthought. The obstetricians have washed their hands of this particular problem.
Perhaps a thought experiment is in order: If we somehow took all the money saved by cutting the cesarean section rate back near the OECD average of 22% (about our 2000 rate), and moving toward midwife-led models and culturally appropriate homebirth care; then we put that money into Aboriginal community-controlled maternity services and women-led healthcare, nutrition, refuge, and family support services: How much good could be done? Why are we as a society so focussed on spending so much money on ridiculously high surgery rates and private hospital stays for privileged women than on the care for those who need it most?
I feel the need to acknowledge here that many ways the people in privileged Australia are very, very lucky to be in a position to be having this conversation at all, because our pregnancy and birthing process is generally very safe (from a mortality point of view). But that doesn’t mean that our maternity care can’t be better, or that the money can’t be far more rationally allocated. Perhaps we could put a proportion of any saved chunk of change into foreign aid with comprehensive women’s healthcare services – oh, wait, that’s banned by Government fiat. Nevermind.
Conclusions
The Review Team concluded that:
* Expanding the range of collaborative care models responsive to local needs will provide greater choice for all women in Australia, including Indigenous women.
* The expansion of collaborative models of care should take account of the successful models for Indigenous women that have been developed in various rural, remote and urban areas.
* Maternity services should acknowledge – and, where possible, accommodate – the particular cultural beliefs concerning childbirth held by many Indigenous families, including a preference for ‘birthing on country’.
* Maternity care health professionals who work with Indigenous women and their families, including those who work in hospital settings, should have appropriate cultural awareness training.
Recommendations
6. That provision of maternity services be considered in the context of all governments’ commitment to close the gap on Indigenous disadvantage, and be developed in partnership with Indigenous people and their representative organisations.
7. In consultation with relevant state or territory governments, that consideration be given to funding expansion of Indigenous maternity care programs, based on current successful models, within a research and evaluation framework.
8. That, in any initiatives that are aimed at supporting an expansion or upskilling of the maternity services workforce, particular focus is given to supporting an increased number of Indigenous people as members of the maternity workforce, across a range of roles.
9. That all professional bodies and employers ensure that all health professionals and other staff involved in the delivery of maternity care receive cultural awareness training.
10. That all professional bodies involved in the education and training of the maternity workforce ensure that cultural awareness training is a core component of their curricula.
4. Information and Support for Women and Their Families
Breastfeeding, apparently, goes here. This section mentions smoking, drinking, and breastfeeding rates. The socioeconomic gap in breastfeeding is mentioned but not explored. The workplace and public policy influence on breastfeeding is acknowledged. Perinatal mortality, perinatal depression, postnatal support all get nods.
But there is a complete absence of anything structural in the recommendations! Where is maternity leave? The WHO Code? Laws to protect public breastfeeding and breastfeeding/expressing in the workplace? Abolishing the GST on breast pumps? The Baby Friendly Hospital initiative? Yet again, as with the Parliamentary Breastfeeding Inquiry, this is all brushed into the too-hard basket.
Instead we get a hotline. Picture me desultorily waving streamers and blowing a limp party whistle.
Conclusions
The Review Team concluded that:
* The need to support women in making informed choices concerning their pregnancy and birthing options is an important issue.
* Women need to be well informed about the risks to themselves and their babies that their decisions may involve. While support services exist, in some instances they could be better integrated with clear referral protocols.
Recommendations
11. That consideration be given to improving the range of birthing and other pregnancy-related information and resources, including those on the internet, that is made available to assist women in informed decision making; with any information materials specifically recognising the needs of population subgroups such as culturally and linguistically diverse communities, women with a disability, Indigenous and teenage mothers.
12. That consideration be given to the establishment of a single, integrated pregnancy-related telephone support line for consumers, possibly as part of the National Health Call Centre, providing both clinical and non-clinical support services, complemented by triage to a number of existing specialised support services.
13. That in order to lengthen the duration of breastfeeding, further evaluation be undertaken to identify the health care or community settings in which breastfeeding information and support are most effectively received, with a particular priority on consulting and supporting women from diverse cultural and socioeconomic backgrounds.
14. That the development of national maternity care guidelines (Recommendation 3 above) consider the Perinatal Society of Australia and New Zealand Clinical Practice Guideline for Perinatal Mortality Audit.
5. The Maternity Workforce
There are shortages throughout. This is a mess. We knew that.
Conclusions
* The Review Team concluded that: Further strategies are required to attract and retain health professionals for maternity services in rural and remote areas.
* Leadership by the professional organisations is vital in encouraging an understanding of the benefits of national cross-professional guidelines for collaborative maternity care.
* Interdisciplinary continuing education activities are an important factor in improving interprofessional collaboration in clinical care.
* Between governments and within the nursing and midwifery professions, issues relating to professional education will need to be addressed for national registration and to facilitate a greater role for midwives in maternity care.
Recommendations
15. That consideration be given to support for the rural maternity workforce to obtain and maintain appropriate training and skills.
16. That consideration be given to identifying the competencies and credentialing required for advanced midwifery practice.
6. Financing Arrangements
6.1 Commonwealth Funding
Private obstetric services were funded by Medicare in 2007-08 to the tune of $211 million. This has increased from $77 million in 2003-04, an increase of 174% in four years. The increase was largely in the form of the newly introduced ‘Planning and Management of Pregnancy’ item, which replaced – or was intended to replace – the “booking fee” paid by insured women to private obstetricians.
Midwifery and Aboriginal Health Worker maternity care has been supported by Medicare, almost entirely in rural areas, to the tune of $457 000.
Fewer than half of the private healthcare insurance services provide any benefits for midwifery care.
Public hospital health care is a major provider also.
Conclusions
The Review Team concluded that:
* Changes to Commonwealth funding arrangements could support the expansion of collaborative models of care, with an expanded role for midwives. Any new Commonwealth funding arrangements would need to be carefully considered to ensure an expanded role of midwives occurred within collaborative, multidisciplinary maternity care models and maintained appropriate quality and safety.
* Importantly, changes to Commonwealth funding arrangements need to occur in a manner that complements the services provided by state and territory governments.
Recommendations
17. That, noting the potential issues to be resolved including the potential interaction with Private Health Insurance arrangements, the Australian Government gives consideration to arrangements, including MBS and PBS access, that could support an expanded role for appropriately qualified and skilled midwives, within collaborative team-based models.
6.2 Professional Indemnity
Private midwives have no access to indemnity cover.
Conclusion
The Review Team concluded that:
Lack of professional indemnity insurance will inhibit the expansion of collaborative models of midwifery care.
Recommendations
18. That, in the interim, while a risk profile for midwife professional indemnity insurance premiums is being developed, consideration be given to Commonwealth support to ensure that suitable professional indemnity insurance is available for appropriately qualified and skilled midwives operating in collaborative team-based models. Consideration would include both period and quantum of funding.
Obvious omissions:
– women with disabilities are only mentioned in terms of needing more “information” (We’ll take accessibility over a website and hotline, thanks!).
– Lesbian women are invisible.
– Non-white non-Indigenous women are subsumed under the bureaucratic header “culturally and linguistically diverse”, and again, are only mentioned in terms of needing more “information” provided.
– I can’t find the word “poverty” anywhere, just a couple of mentions of “socioeconomic status” as a “risk factor”.
So, what do you think?
Categories: Culture, gender & feminism, health, indigenous, medicine, Politics, social justice, Sociology


Now, do I dare read the news?
I haven’t really elaborated on my disaste for the emphasis on “collaborative care” in this post. My main objection is that it’s just bureaucratic code for more of the same: “obstetrician-led care” with a few tweaks. It’s just slapping a pretty label onto the same old concepts. It doesn’t encompass true independent midwifery-led care, nor is it woman-centred in any way. The “collaboration” is between doctors and nurses or midwives, not healthcare practitioners and women. Bleagh.
Looking at those figures it’s pretty easy to see that cutting down the caesarean rate and weaning people off the belief that having private a OB birth your baby is automatically the safest and best option would save the govt a lot of money, which it could put to good use – as you noted Lauredhel. I find it horrifying that the medicare payments to OBs went from $77 mil to $211 in less than five years.
This.
I haven’t read the report myself – did it mention the impact of the monumental increases in professional indemnity insurance on those costs of private OB? One of my hobby horses is that compensation and liability need to be divorced. Something really bad happens and you deserve compensation – you get it, regardless of whether there was really any negligence. You are negligent – you pay appropriate fine regardless of whether anyone got hurt. This seems particularly relevant in the whole birth business, since when shit happens, the results are devastating for everyone involved, which can easily translate into massive legal cases. If professional indemnity is offered to midwives, it is highly likely to just make them even less affordable under the current system.
I had a private OB for all of my (successful) pregnancies, and the thing that annoyed me was that I really felt there was benefit for the pregnancy, but none at all for the delivery. Well, except that someone needed to be able to say “yes” when I asked for pethidine, and currently midwives can’t do that.
But Yay! for the recommendation for more birth centres. I was lucky enough to have 2 of mine in one, and they are a wonderful institution. Those midwives (who did half of my prenatal care as well) were amazing, beautiful individuals.
Ariane’s last blog post..Distractions from a previous life
The majority of Indigenous women who are considered “at risk” pregnancies (pretty much all women who have not had antenatal care, live in remote areas, Indigenous teens, or who (in some cases) want to birth at KEMH), give birth at King Edward Memorial Hospital, the womens’ and infants’ teaching hospital in Perth. This makes the general obstetricians’ standpoint on culturally diverse maternal care all the more galling for its disingenuous stance on rigorous maternal care more broadly. I think you are right to highlight the disparity in maternal care the ‘establishment’ medical profession is apparently willing to accept for Indigenous and non-Indigenous women. I don’t however hold out for a logical or evidence-based response.
I also think the AMA and Dr Capolingua in particular need to be taken to task over this. Either the AMA stands by its preference for obstetrics-attended birthing in the interest of patient safety, or it should be held to account for obstetricians’ apparent washing their hands of Indigenous women in remote (and ‘undesirable’) practice locations in preference for midwives and community-controlled birthing options. There is indeed a disconnect between the two.
PS I’ve amended my screen name to distinguish between the other person who uses Rachel as a screen name. I did not know she was using this screen name, otherwise I would’ve adopted a non-name alternative for myself.
I find that Monty Python sums it up pretty well for me (from a priviledged white birth perspective.)
https://www.youtube.com/embed/lxOu1DyVQV8?version=3&rel=1&fs=1&showsearch=0&showinfo=1&iv_load_policy=1&wmode=transparent
It’s been a very strange component of the getting pregnant/birthing/mothering thing to find myself wanting to scream at Health Minister(s) “I want to SAVE YOU MONEY by having babies at home with a midwife” and being told “NO. NOT UNDER ANY CIRCUMSTANCES” over and over again. I think I lost all hope when the Women’s (in Melbourne) closed their FBC.
Great post, Lauredhel. Thanks for all the time and energy. Just a few things that I’d like to say.
Ms Bryant may not be a midwife, but I’m sure she has staff who are. She didn’t write the report herself, personally, her staff would have done that, although of course she’s responsible for errors (including the ones you’ve picked up.) To be fair to her, this office has only existed for five months (that’s right, we didn’t even have a Chief Commonwealth Nurse/Midwife until then – it’s a Rudd govt invention). In that time frame it’s a bloody miracle this report has even been scoped, let alone completed.
Maternal mortality has been reported as peri-maternal deaths since, well, forever. There are no figures showing the deaths of women directly from pregnancy, because that’s not how they are collected. Maybe they should be, maybe they will be, but they haven’t been, and Ms Bryant can’t report figures from the past that don’t exist. I agree that the legend on that graph is misleading; writers have assumed that readers understand how the figures are collected.
I think you make some excellent points about more work needing to be done on differentials for disabled, Indigenous and poor women. I wouldn’t rule out the possibility of another report which looks at these things in more detail, now we actually have an office that can look at these things. I’m not sure that pregnancy and birth are any different for lesbian women, though (apart from the issue of actually getting pregnant in the first place! 🙂
Disclaimer: I don’t have any connection to Bryant or her office, but my partner is a person who takes a close professional interest in these things, and is also a professional researcher. We discussed the report briefly a few days ago, but she hasn’t had any input into what I’ve just written; we didn’t have time to talk this morning. If she has anything to add I’ll encourage her to comment too.
M-H’s last blog post..A boost to the ego
M-H: “Maternal mortality has been reported as peri-maternal deaths since, well, forever. ”
I’m a bit lost on what you mean by “peri-maternal deaths”, M-H, and I’m not finding that phrase anywhere amongst WHO/ICD-10 definitions. Could you explain, please? (Section 2.1 here gives some standard definitions, if you’d like to know where I’m coming from.)
I’m also not sure what you mean by “writers have assumed that readers understand how the figures are collected”. I’m surely in the intended audience of the report, yet I found it confusing – it left me wondering whether they had somehow managed to collect data for deaths in childbirth, and I searched the report for some evidence of this, and how it was defined. It took me some time to figure out what (I thought) they really did mean.
Sorry. I meant ‘deaths of women that occur within a certain period before or after giving birth, no matter what the cause of death’. The different causes of death have always been lumped together as ‘maternal mortality’ and it wouldn’t be possible to go back in history and untangle the reported number into its constituent causes. And to the second point, I think that the writers were assuming that the readers would know how the maternal mortality stats were collected and what they did in fact reflect. Thus they carelessly labelled their graph, not realising that readers would take them as literally as you (quite reasonably) did.
M-H’s last blog post..A boost to the ego
I wonder what else they carelessly labelled something else, figuring that we’d Just Know what they really meant?
Not all maternal deaths are just lumped together in Australia as “maternal mortality” without any further granularity – are you aware of the detail in the maternal mortality reports? Here’s one example.
That’s a recent report (and an interesting one). If you’re trying to compare today’s figures with older ones you have to use the same set of stats. For a long time this work of breaking down the maternal mortality statistics wasn’t done, as no-one thought it was important enough. amking out that having babies was risky has been a good way to keep women dependent on (mostly male) gynaecologists rather than on (mostly female) midwives.
Look, I agree that the use of that graph in that way was misleading. but I’m just glad that the work is being started. It’s certainly not finished.
M-H’s last blog post..A boost to the ego
So after the violent birthrape, the subsequent HRC complaint, and the hiring of an independent midwife for baby4, I was looking forward to the release of this review. I was shocked Tuesday when my middie told us that midwives who attend homebirths after July 2010 will be de-registered. Is this the case? I’ve not read the report. If this is true then Australia is moving away from the NHS (UK) which provides for homebirth, and closer to ACOG (US) which wants to outlaw birth at home.
Am I missing something here? Since when is the Commonwealth allowed to whore out private citizens to appease corporate and (S)OB appetites? Are we being compensated for our “services” with the baby bonus? Or could this really be about establishing a no-fault system for bad practitioners to hide behind in exchange for some small movement toward following legislation requiring valid consent and maybe even evidence based medicine (which includes midwives)?
And, according to figure 2, infant deaths have increased between 2001-2006. The 2nd leading cause of death of infant deaths, as the first is congenital malformation, is intrapartum asphyxia, meaning lack of oxygen during the immediate period surrounding birth. More syntocinon anyone? Plus RANZCOG is advocating the use of Cytotech or misoprostal for induction and augmentation in births- including VBAC. So, more interventions, dangerous drugs, and an increase in fetal death. Yep, it’s all about safety.
Does anyone think that this report exists to increase the power of obstetricians? I think that’s unlikely. The most important thing about it, in my view, is that it is the first one from the new office of Chief Nurse and Midwife. Not from the AMA, not from RANZCOG, not from Commonwealth Medical Officer or any of the doctor’s lobby groups. This is the first report that has been funded from a government department that is run by nurses and midwives. That’s got to be a good thing, doesn’t it?
M-H’s last blog post..You can’t get builders like you used to…
I don’ think so MH, but I am concerned that it doesn’t adequately address women’s wants and needs when it comes to woman centred birth and options available for birthing with a midwife either in a birth centre or at home. It’s still a bit – we know what’s good for you so shut up and get on with gestating and we’ll get the baby out when we are ready.
A good thing? This may very well be a good start, but at this moment I will reserve judgement. To blindly believe that the collusion that currently supports the hospital system – with nurses and midwives participating in, and cow-towing to, OBs flagrantly disregarding legal requirements and best practice – is not also at play in this review, is the kind of thinking that would lead me to choose the same doctors and hospital for this pregnancy. Just not gonna happen. Furthermore, if homebirth midwives really will be de-registered after July 2010 to appease the AMA and RANZCOG, and apparently hospital nurses and midwives, than this review directly increases the power of hospitals and OBs.
My partner is a research scientist, has looked at the stats., and is mad as spit that this review is splitting the option of privately birthing at home off from other places of birth with qualified practitioners, while simultaneously claiming to increase choices. This new office can only be a good thing IF it is truly independent, and frankly, leaving homebirth off the list of goodies for girlies does not indicate that that is the case. And when I finish my legal degree……….
It’s true. Homebirth will be illegal as of July 2010.
Hello Labor party who we voted for for the first time because maternity care in this country is crap regardless of what AMA and RANZCOG has to say. We will not vote for you again if you outlaw homebirth! The NHS is supporting HB and HBAC so what’s the go here?
Nicola Roxon, I see from old media releases that you are acquainted with Andrew Foote OB, former AMA president. What interesting company you’re keeping. What has become of him I wonder as he hasn’t said a word about this review publicly and he was so vocal before. Lawsuit got his tongue?
Just to be more accurate about this: on the information we currently have available, if the path continues now as it seems is planned, attending a homebirth as a midwife may be illegal as of July 2010.
This issue revolves around the National Registration scheme, which you can read more about here at the Australian College of Midwives. If midwives are forced to practice only when they have indemnity insurance, and indemnity insurance excludes homebirth, obviously attending a homebirth as a midwife will be illegal.
Unfortunately, the College of Midwives seems to only address the positives of the scheme for midwives, and not the negatives. I sincerely hope that their members are lobbying them strongly for more accurate information on the issue.
I have seen no formal moves toward making it illegal for a woman to birth at home; only moves to make it increasingly difficult for women to do so readily with an attendant of their choice. Which, one might argue, has much the same effect. I predict there being moves toward establishing a network of underground homebirth attendants, just as there have been networks of underground abortion practitioners wherever abortion was made inaccessible. Unfortunately, this will continue to make homebirth increasingly inaccessible for the majority of women, who will see it as a dangerous “fringe” practice. And these perceptions of homebirth may make it increasingly easy for less informed child protection officers to demonise certain mothers.
I have not bothered to read the entirety of this article.
[Mod note: I have not bothered to post the entirety of your comment. ~L.]
So good to see your comments Lauredhel.
I am one of the independent midwives in Victoria facing loss of my livelihood if the recommendations of the Review are implemented. I have linked this blog to mine http://villagemidwife.blogspot.com/ where I have made comment about this and other maternity issues. Also your readers might want to check http://midwivesvictoria.blogspot.com/ which is the Midwives in Private Practice (MIPP) blog – also managed by yours truly. Most of my colleagues are keeping quiet. Perhaps it will go away!
I find the Report wishy washy and lacking any direction other than backward. The Discussion Paper advised that: “Improving the delivery of maternity services in Australia is not the responsibility of any single party. While there are actions which could be undertaken by the Australian Government on its own, substantial change requires a combined approach.”
Let’s get real. Most of the Recommendations could be done without the Australian Government’s permission. The Minister has the opportunity to move the focus of maternity care from a broken system, and a financial monopoly privileging the medical profession, to the woman, by funding a woman to obtain the basic care she needs. Yet from the Report, and the Minister’s statements on the SBS Insight program on Tuesday night, she seems unaware that if she follows the advice of the Recomemndations she will be setting birth back into the doctor supervision era that most midwives remember. It was only 1996 when Victorian midwives were free of the old regulations (1985) that required us to have a doctor’s permission to do a vaginal exam. Whose vagina, you may ask?
Joy Johnston’s last blog post..LACK OF INSIGHT
This is clearly a very heated issue for many women who feel (and rightly so) that rights and choices are being stripped from them.
It is important, however, to maintain some perspective in response to the review. Angry and often poorly framed criticisms won’t help bring balance to the system. A review can only draw on available data, and I realise you have mentioned a few sources it overlooked. The reason the medical fraternity has so much pull, is that it is backed by evidenced based research (whatever the quality of that research might be, and I am certain it varies dramatically), which is highly regarded by people who have to weigh up risks. Nobody wants to be held responsible for making a decision which could end in disaster because they ignored evidence.
My point here, and it applies to all “fringe” practices, is that to get a piece of the funding pie you need to have facts and figures not angry rants.
I apologise if this belittles the issue, which I certainly do not wish to do. I view women’s rights to choice as very important. I am a woman and I do not appreciate being told what decisions I need to make.
I support you in your fight to practice your trade, but perhaps counter the report with an evidenced based report of your own.
There is a huge amount of evidence-based information out there, yhs18, on this blog and elsewhere. Follow the Related Posts, follow the links in them and further Related Posts, and see where you end up. Look for my posts on the Fortelesa Declaration, and Cochrane Review on midwifery led care, and the Related Posts from there; and look for more recent studies on homebirth safety which have even been all over the mainstream media. Look for the stats I’ve posted on Western Australian birth statistics. It’s not all on this one page; you’ll have to click a few times. There you will find that surgical obstetrics is _not_ working from the evidence base, no way no how, and that even some surgeons are starting to realise that. Unless you really truly believe that over 50% of births need to involve surgery and over 75% require major intervention; if you do believe that, there’s probably nothing I can say that will change your mind.
Tone arguments about “anger” are unhelpful and will not gain you allies here. Please don’t use them against feminists in this space again. We’re angry because we’re paying attention. Women and midwives are being criminalised here.